Move over COVID: Monkeypox forces new public health test on state, local governments
Experts point to steps health departments and others can take to meet the challenges posed by the spreading disease.
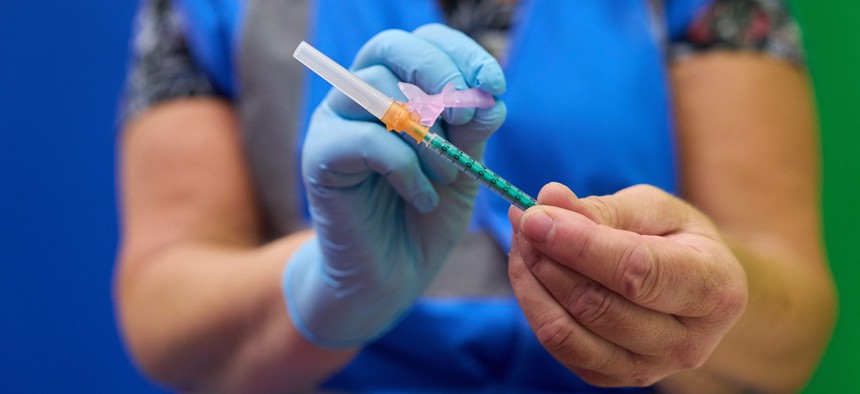
A health care worker prepares a monkeypox vaccination shot in the Netherlands, July 25, 2022. Photo by PHIL NIJHUIS/ANP/AFP via Getty Images
As monkeypox cases rise across the country, health officials are moving to address the infectious disease while also dealing with the ongoing fallout from the COVID-19 pandemic.
The tandem outbreaks present a unique set of challenges, especially for a public health workforce worn down by over two years battling the coronavirus. But experts say there are some clear cut actions authorities can take to address the spread of monkeypox, particularly when it comes to communication with the public and ensuring health professionals have the information they need.
The disease, which is rarely fatal, causes a rash that appears similar to pimples or blisters, and can also cause symptoms like fever, headache, chills and exhaustion. On Saturday, the World Health Organization declared the monkeypox spread a global health emergency as the disease has appeared in several countries where it isn’t normally found, including in the United States.
As of July 25, there were 3,487 monkeypox cases reported in the United States, according to the Centers for Disease Control and Prevention. In Florida as of the same date, the state's Department of Health reported a total of 310 confirmed or probable cases in 17 of the state's 67 counties, with the most – 151 cases – in Broward County.
Dr. Aileen Marty, an infectious disease expert with Florida International University, told South Florida's WLRN that "fortunately most of the cases that we've seen in the United States have been mild. ... We have actually several different antivirals. We even have some drugs that were developed for herpes that work well.
"Unlike COVID, we're not starting from scratch," she added. "We've known of this virus for a long time. Yes, it's a little bit different, it seems to be a little more eager to spread person to person and that's a problem, but we do have a vaccine that works." (The World Health Organization this week said vaccines used during the smallpox eradication program also provide protection against monkeypox.)
Added Brian Castrucci, president and chief executive officer of the de Beaumont Foundation, a public health nonprofit: “ ‘Outbreak,’ because of the way that we use the term, always comes with fear and trepidation. That doesn't have to be [the case]. We can have a thoughtful, measured response that allows us to control the virus as much as possible, and limit the damage that it can do.”
Now is the time for a concerted effort to ensure that local health departments and providers have the information they need to recognize and treat monkeypox, Castrucci said: “We have to meet this health care and public health workforce where they are and not rely on them to go out and look for this information."
Communication is key right now, Castrucci added. He noted communication missteps during the Covid-19 response and said public health leaders can draw from those mistakes as they work to inform citizens about monkeypox. “They need to really be thoughtful in their communication, be accurate, and be consistent and acknowledge changes. Sharing that with the public in a transparent way is really important,” he said.
Through the Covid-19 pandemic, many local health departments sought to improve public outreach by strengthening their communications staff, according to Adriane Casalotti, chief of government and public affairs for the National Association of County and City Health Officials.
“It's so important that their community–and decision-makers in their communities–know what the situation is and what role they can play in stopping or slowing the spread,” Casalotti said.
Casalotti explained that, so far with monkeypox, municipalities are generally falling within three categories.
The first are places like Los Angeles and New York, where there are many reported cases. In those cities, there’s a lot of public-facing activity: vaccinations, community outreach, provider outreach, and case investigations to learn more about who is at risk of infection.
At the other end of the spectrum are communities that don’t have any reported cases and are far from areas where infections are emerging. In those places, much of the action is happening behind the scenes as health departments, community organizations and health care providers learn about what to look for, and if there is a case, how to care for and monitor the infected person.
Then there are areas that fall somewhere in between. They have few or no cases, but expect to see more soon. Those areas are also ramping up their community and provider education efforts, as well as ensuring there are robust pathways for testing.
“It's kind of a wide range, but no matter the community," Casalotti said, "they have a role to play.”
Unlike the early days of Covid-19, when there was little known about the new and deadly coronavirus, public health officials are more up to speed on monkeypox and more accustomed to responding to outbreaks of this sort, Casalotti said.
Even so, there are difficulties, including a shortage of the vaccines that can be used against monkeypox.
There aren’t enough of one type of vaccine—known as JYNNEOS—to meet demand, Casalotti explained, and another—ACAM2000—can have strong side effects and isn’t suitable for many people, including those who are pregnant, those who are immunocompromised, and those with preexisting health or skin conditions.
Burnout in the public health workforce is also a problem. After two and a half years of being battered by the Covid-19 health crisis, public health and health care professionals are exhausted, Castrucci said.
In a survey conducted at the end of last year, more than a quarter of public health employees said they were considering leaving their organization, and 44% said they are planning to retire or leave for other reasons in the next five years. Of those, 76% said they started thinking about leaving after Covid-19 struck.
Now, health professionals again find themselves in a position where they will have to guide Americans through the response to an unfamiliar and infectious disease. Castrucci said he’s not sure what the pandemic-fatigued public’s tolerance will be for listening to them.
To avoid a worse outbreak, he said, health officials need to follow the “well-proven” steps of outbreak investigation and control. “We know how to do this. We have people trained to do this,” Castrucci added. “Now we just have to let them do their job.”
A version of this story was originally published on Route Fifty.
NEXT STORY: State moves ahead with rulemaking on contentious new 'Parental Rights in Education' law
